
Sometimes a person with a drug addiction may have tried many different approaches only to find that they still cannot overcome their addiction. Today, a significant group of scientists and addiction specialists uphold using Electroconvulsive Therapy (ECT) in the most severe of these circumstances.
History Of ECT
Electroconvulsive Therapy, or what was once called Electroshock Therapy, has been around for some time. ECT was initially and most widely used as a treatment for various psychiatric conditions. It was not until fairly recently that it garnered wider support as a method for fighting addictions.
Intensive ECT has been around since 1946 and since then many changes for the better have been made. Admittedly, for some, Electroconvulsive Therapy may yet have an unfortunate stigma attached to it; this is largely due to misinformation about the current treatment module verses that of many years past. It is important to realize that though—at the time—these concerns were well-founded, today, the circumstances and results that they were based upon have been significantly altered and improved, making the treatment safe and far more effective.
In the past, people would undergo the treatment without assistance from anesthesia or medications. Due to the intensity of muscle spasms and seizures, these methods often resulted in broken or dislocated bones, fractured teeth, or cognitive impairment. Today, this problem is alleviated by the introduction of anesthesia and medications such as muscle relaxants which curtail previous damage and risks.
Medscape reports that today, roughly 100,000 people use ECT within the United States. This number is a total and is not limited only to those who received the treatment for addiction. Currently it has been found to be most successful when paired with medicatio. This pairing lends to greater efficacy for more permanent and long-lasting results.
What Scientific Studies Show
Though ECT is recognized as an effective method of treatment of mental illness by the American Psychiatric Association (APA), the American Medical Association and the National Institute of Mental Health, research is currently ongoing in the realm of addiction studies. This treatment, used in worst-case scenarios for severe and otherwise untreatable addictions, has been used as treatment protocol with successful results and is supported by scientific studies.
One study published by the National Institutes of Health (NIH) was based on the selection of six individuals that had “a history of addiction unresponsive to previous forms of therapy, showing a downhill course, and an apparently poor prognosis.”
The treatment consisted of the multiple shock method over a period of 4-6 weeks with participants undergoing a closely monitored, supervised withdrawal which was supported with doses of chlorpromazine. They then received both the medication and the ECT in tapered doses for six months, eventually to the point of ceasing both. After a period of 2-5 years, 4 out of the 6 participants remained successful within their sobriety and recovery.
The study makes an interesting point: “drug addiction and psychotic illness both show a pattern of irrational activity and also a persistent activity or drive which is both detrimental to the organism and very hard to change.” Though scientists don’t yet understand why, they do know that ECT does, on a biochemical level, alter the chemical infrastructure that might be responsible for these harmful patterns and self-destructive tendencies.
A second study published in Frontiers in Psychology found that “human studies indicate that ECT leads to dopamine system activation… the impact upon the dopamine system is corroborated by findings of dopamine receptor changes.” Dopamine is vastly interconnected with many types of drug addiction, hence the possibility that these changes brought about by ECT may have something to do with its efficacy.
Who Should Consider ECT?
Electroconvulsive Therapy is not for everyone and it is not a decision that should be made lightly. This procedure should only be used under the advisement of a knowledgeable physician that has an in-depth understanding of an individual’s situation, treatment history, and addiction. It should only be used as a last resort for patients that have been unable to cease their drug use under any other form of treatment, including behavioral therapy, medications, or a combination of both.
A person should only choose this route if they thoroughly understand the risks and side effects along with the benefits. A person and their family or support system should take ample time to review and consider all the information that their medical and addiction team presents to them in order to make an informed decision before they consent to this procedure. Be honest and take the time to voice any questions or concerns that you might have to your care team.
It is important to remember that this may not be fully curative, as The APA, who states “most people treated with ECT need to continue with some type of maintenance treatment. This typically means psychotherapy and/or medication or, in some circumstances, ongoing ECT treatments.” This does not mean that the treatment is not worthwhile, again, as this treatment can provide hope and alleviate the toll of an addiction for a person who is downtrodden and physically and mentally in danger after not finding success in any other treatment.
How Does ECT Work?
The Mayo Clinic defines ECT as “a procedure, done under general anesthesia, in which small electric currents are passed through the brain, intentionally triggering a brief seizure.” Small electrodes placed at specific points against your scalp are responsible for delivering these brief electrical pulses, each of which lasts approximately 20 seconds to one minute.
Research illustrates that each treatment should be set apart by at least a day. The amount of treatments may vary depending on how well and how quickly a person reacts to them. Mayo Clinic states that “ECT treatments are generally given two to three times weekly for three to four weeks — for a total of six to 12 treatments.” Depending on the person, some people may require maintenance treatments afterwards.
ECT treatments alter your brain chemistry in a manner that produces desired effects. Though the exact mechanism by which this occurs is not entirely known or understood, what is known– as Medscape reports –is that “ECT affects multiple central nervous system components, including hormones, neuropeptides, neurotrophic factors, and neurotransmitters.” All of these are involved within the physiology of an addiction.
Prior to treatment a person must undergo a thorough medical and physical assessment, including a careful review of medical and addiction history, including any previous treatments or medications, a physical, blood work and/or other laboratory tests, and an electrocardiogram. Patients should discuss any and all medications they are taking, as Medscape recommends that “benzodiazepines should be lowered in dose or discontinued if possible” for the treatment. It is also often recommended that patients discontinue use of any MAOIs.
Medscape cites the following as essential steps within the evaluation:
- A thorough psychiatric history and examination, including history of response to ECT and other treatments
- A medical history and examination, with special attention to cardiovascular, pulmonary, neurological, and musculoskeletal systems
- A history of dental problems and examination for loose or missing teeth
- A history of personal and family experiences with anesthesia
- A cognitive assessment (at minimum, evaluation of orientation and memory)
The procedure may be done in either an inpatient or outpatient setting. The treatment itself is fairly quick, the majority of time being spent within a treatment session being taken up by the preparation and recovery time. During the procedure the medical team will maintain constant monitoring of a patient’s vital signs. Due to the anesthesia, the procedure will not be recalled by the patient and, being performed under general anesthesia, all patients must have an accompanying party present to drive them home afterward.
Does ECT Work?
Yes, it does, though there is some variation as to who ECT works on and to what extent. Scientists are still learning about the intricacies of the treatment and how it applies to addiction rehabilitation. The Royal College of Psychiatrists states that ECT does “change patterns of blood flow through the brain and change the metabolism of areas of the brain… recent research has also suggested that ECT can help the growth of new cells and nerve pathways in certain areas of the brain.” This is of great relevance to those suffering from an addiction as drugs can actually inhibit certain neural functions, processes, and even cellular growth.
More is understood about how ECT works to treat mental health concerns that may accompany addiction, such as major depressive disorder, than as a tool within addiction treatment. This holds additional relevance for those that may have a dual-diagnosis. Depression is often linked to addiction as a co-occurring disorder, thus the possibility that a person may experience an alleviation of both conditions, enhancing the chance at obtaining and maintaining sobriety while avoiding the complications of relapse.
This treatment is beneficial to those who find themselves having exhausted every other option of rehabilitation or for those who are in need of immediate help due to the fact that their addiction is so severe that it is seriously endangering their mental or physical health. Some people, despite the fact that they desperately want to resolve their addiction, find themselves caught in a continuous cycle of addiction and relapse. This treatment, in its intensive nature, is specific in helping said individuals.
What Are The Risks Of ECT?
Although ETC is much safer today, it is not without risks, some of which are not yet fully understood. There are still some people, including medical professionals who are stand against this treatment for a variety of reasons.
If the patient has a history of osteoporosis or any spinal injuries needing to be evaluated, and if he is deemed fit for the procedure, he’ll need to be suitably medicated as to not cause further injury by way of the physical manifestations of the seizures. Patients with a history of aneurysm and stroke may be advised to avoid this procedure due to the excess of pressure and blood flow within the cranium. If someone has a history of hypertension, he will need to receive medicine to stabilize the condition prior to beginning treatment.
This treatment holds the same risks that any procedure that includes general anesthesia carries. After treatment, the individual may experience a small level of discomfort, including, but not limited to confusion accompanied by minor memory loss, fatigue, nausea, jaw pain, muscle ache, or headache. These side effects may last only a matter of minutes or extend for several hours.
The most common side effect is short-term memory loss, which often occurs in memories that were made within a certain period of time prior to the treatment (typically within a matter of weeks, though in some cases longer). In other instances, a person may forget events directly following the treatment. In either instance, time usually resolves these things, however, in the worst case, this may last longer or even cause permanent memory loss. Some patients do report even in years following that their general memory functions aren’t as good as they were prior to the procedure.
JAMA Psychiatry published a study in 2009 that focused on the role of ECT within treatment for depression. Though not in direct relation to addiction, we can nonetheless extract some useful information from the study, including that of potential side effects. In this report, of 750 patients, “a single adverse event was experienced by 22 patients, 5 had 2 adverse events, 9 had a serious adverse event, and 2 experienced both an adverse event and a serious adverse event.” It went on to say that “the most common adverse event was a cardiac complication… typically manifesting as sustained tachycardia and/or hypertension after seizure termination.”
Stay Educated And Get Help Making An Informed Decision
 It is important when making the decision to receive ECT as a form of addiction rehabilitation, that you weigh the pros and cons. Consider the damage and risks that may continue or result if you do not intercede or receive help, versus the considerations and results of the treatment.
It is important when making the decision to receive ECT as a form of addiction rehabilitation, that you weigh the pros and cons. Consider the damage and risks that may continue or result if you do not intercede or receive help, versus the considerations and results of the treatment.
It can be overwhelming to deal with an addiction and it can be even more daunting trying to wade through all the information and choices that revolve around choosing treatment. It isn’t something you should do alone, which is why we’re here to help. At DrugRehab.org, we have professional and compassionate counselors standing by to help you with any questions or concerns you might have about the road to recovery and possible treatment options. Don’t hesitate to contact us today and begin on your journey to a healthy, happy life!


 Overall, benzodiazepine use was almost twice as prevalent in women as it was in men. This could be due to a wider social acceptance of women speaking with a psychiatrist about emotional issues than men, however it could also be linked to other environmental factors.
Overall, benzodiazepine use was almost twice as prevalent in women as it was in men. This could be due to a wider social acceptance of women speaking with a psychiatrist about emotional issues than men, however it could also be linked to other environmental factors.



 As previously mentioned, the Brompton Cocktail consists of a few different substances, meant to give ultimate relief from pain. Traditionally, the Brompton Cocktail consisted of morphine or
As previously mentioned, the Brompton Cocktail consists of a few different substances, meant to give ultimate relief from pain. Traditionally, the Brompton Cocktail consisted of morphine or 
 Treatment for any type of addiction has to be comprehensive. Addiction doesn’t just affect your physical health, but actually changes the way you think and behave, so treatment for it must address these changes and work to better them. This is especially true when dealing with addiction to more than one substance.
Treatment for any type of addiction has to be comprehensive. Addiction doesn’t just affect your physical health, but actually changes the way you think and behave, so treatment for it must address these changes and work to better them. This is especially true when dealing with addiction to more than one substance.









 For Treatment Of Opiate Addiction: For those that suffer from opiate dependence, this drug is used as a part of medication-assisted treatment (MAT) or therapy to help people taper off opiates. Buprenorphine binds to and occupies the same opioid receptors as the abused drug, creating the same effects. It is for this reason that cravings are reduced. Like any opiate, buprenorphine works on the Central Nervous System, but in this case it causes decreased withdrawal symptoms.
For Treatment Of Opiate Addiction: For those that suffer from opiate dependence, this drug is used as a part of medication-assisted treatment (MAT) or therapy to help people taper off opiates. Buprenorphine binds to and occupies the same opioid receptors as the abused drug, creating the same effects. It is for this reason that cravings are reduced. Like any opiate, buprenorphine works on the Central Nervous System, but in this case it causes decreased withdrawal symptoms.
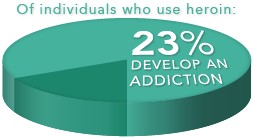 In the United States, an
In the United States, an  In light of the staggering rise in heroin usage in the United States, researchers have resolved to find alternative methods of relief.
In light of the staggering rise in heroin usage in the United States, researchers have resolved to find alternative methods of relief. 






