What Is Heroin?
Heroin is an opioid drug processed from morphine. In its pure form, it’s a white, bitter powder. The pure form is mainly smoked and snorted, as explained by the National Institute on Drug Abuse (NIDA). Powdered heroin is commonly cut, or adulterated, with other substances. When this occurs, the color of the drug changes, taking on a brownish tint.
Heroin is also found in another form called black tar heroin. The appearance is as the name suggests, thick, dark colored and either sticky or hard. The color and form occur from the impurities which result from the manufacturing process. Due to the impurities and lesser quality, many injection drug users choose to inject black tar.
How Does Heroin Work?
Opioid drugs work on your body and brain by attaching to opioid receptors. When this occurs, you experience a pain-relieving effect. Recreational drug users seek to induce another feeling from this chemical brain stimulation.

Heroin, like other opioids, creates an intensely pleasurable state of euphoria. It can also create what is termed a rush. Heroin depresses your central nervous system (CNS). This is one reason why it’s such a dangerous drug.
What Are The Signs Of Heroin Use?
Learning the signs of heroin use can help you to identify a person in need of help.
When a person uses, they may experience:
- A “rush” and sense of euphoria.
- Decreased pain.
- Dry mouth.
- Flushed and warm skin.
- Heavy limbs.
- Intense drowsiness and wakefulness (being “on the nod”).
- Intense itching.
- Nausea and vomiting.
- Slowed breathing and heart functions.
If any of these seem familiar, don’t hesitate to speak up. It can be hard to have this conversation, but by doing so, you could be saving your loved one from harm and even death.
The Risks And Dangers Of Heroin Abuse
If you’re a heroin user or know someone who is, it’s pertinent you understand the risks and dangers of abuse. This information could help to save your life.
Here are some general dangers linked to heroin abuse:
- Addiction
- Compromised immune system
- Complications of the lungs, including pneumonia
- Decreased memory and decision-making skills
- Endocarditis (infection of the heart’s lining and valves)
- Impaired verbal and cognitive functioning
- Poor impulse control
- Miscarriage
- Risky sexual behaviors
- Withdrawal
Heroin can cause overdose, even on the first dose. Overdose occurs because your CNS becomes severely depressed. This leads to drastically reduced heart functions, blood pressure, and breathing rates. The intensity of these factors can cause coma, permanent brain damage, and may lead to death. The CDC reports that heroin-related overdoses are on the rise. Between 2002 and 2013, they rose 286 percent.

What Ways Do People Administer Heroin And What Are The Risks?
As previously mentioned, people choose to use this drug numerous ways. In addition to the above, each route of administration has specific signs of abuse and unique risks.
Injecting Heroin Intravenously (IV)

To prepare for injection, the user liquefies and dissolves the heroin by diluting and heating, or “cooking” it. It is then loaded into the syringe. Shared needles increase the risk of transmissible diseases, including HIV/AIDS and hepatitis B and C. Injection can also cause abscesses, track marks, and other infections within certain soft tissues.
When many people think of injecting heroin, they are quick to think of intravenous (IV) drug users. This means that the drug is injected directly into the vein. Before a person can do this, they tie off their arm with a piece of rubber tubing or a belt to make their vein bulge. These individuals also inject the drug at various other locations throughout their body, including the leg, neck, feet, and even groin.
Intravenous injection allows any contaminants or cutting agents within the heroin to travel throughout the bloodstream. This can lead to:
- Clogged vessels
- Cellular infection or death in certain organs
- An immune response which can cause arthritis and similar illnesses
According to NIDA, IV heroin abuse can cause:
- Collapsed veins
- Scarring
- Necrotizing fasciitis (sometimes referred to as flesh-eating bacteria) causes tissue death
Heroin can also be injected into into the muscle (intramuscularly) or directly beneath the skin (subcutaneously or “skin popping”).
Smoking Heroin

Users place the heroin (typically black tar) on aluminum foil or the top of a pop can and heat it with a lighter. They then inhale the vapors with a straw or hollowed out pen. This is referred to as “chasing the dragon.”
The University of Arizona outlines the following dangers of smoking heroin:
- Pulmonary (lung) function becomes compromised
- An uncomfortable shortness of breath (dyspnea)
- Severe and repeated asthma attacks (status asthmaticus)
Smoking heroin can also cause leukoencephalopathy, a serious disorder of the CNS’s white matter. A debilitating disease, it causes parts of your brain and spinal cord to deteriorate. This can lead to slurred speech, vision loss, paralysis, and even fatalities.
Sniffing/Snorting Heroin (Insufflation)
These methods are sometimes referred to as insufflation. To prepare, users draw the drug into lines with a razor or credit card on a hard surface like a mirror. They then use a straw, hollow pen, or rolled dollar bill to inhale it into their nasal cavity. This method is very invasive. It can cause great damage to the nose and surrounding areas, including:
- Bone loss
- Creating a hole in the septum (area between your nostrils)
- Chronic nosebleeds
- Collapsed nasal passages
- Constant runny nose
- Perforation (hole) in the roof or back of your mouth
- Saddleback nose (a broad, flattened nose)
According to the Center for Substance Abuse Research (CESAR), sniffing the liquified version of heroin through a nasal spray bottle is called “shabanging.”
Mixing Heroin With Other Drugs
Heroin is commonly abused with cocaine (including crack). Alternately snorting lines of these drugs is called “crisscrossing.” If a user injects them both at once it is called “speedballing.” Both of these methods are highly dangerous, as heroin is a depressant and cocaine is a stimulant. Because of this, your body and brain are being simultaneously pulled in two different directions. This increases your risk of overdose and death.
As the opioid epidemic increases, heroin is increasingly used in combination with other, more potent, opioid drugs. Responsible for countless overdoses, these deadly concoctions include fentanyl and carfentanil, and as of late, the lethal mystery combination termed “grey death.”
Some individuals purposely seek out these combinations, believing that they will increase their high. Others stumble into using them, as they unknowingly purchase heroin that is cut with these drugs. By either path, these powerful opioids have left a wave of destruction and overdose deaths across our nation.
Start Living A Drug-Free Life
No matter how you abuse heroin, you’re putting yourself at risk for addiction. Is heroin taking over and ruining your loved one’s life? Or maybe you’re the one struggling. Either way, we can help. It is possible to beat a heroin addiction and find sobriety. DrugRehab.org knows how to find the best heroin rehab centers for your needs. Contact us now.
For More Information Related to “How Do People Use Heroin?” Be Sure To Check Out These Additional Resources From DrugRehab.org:
- How Do People Become Addicted to Heroin?
- Snorting, Smoking, or Injecting Drugs: Which Gets You Addicted
- The Dangers of Snorting Oxycontin (Oxycodone)
- Heroin and Opioid Addiction Statistics
- The Most Commonly Abused Opiates
- Opiate Epidemic Is Changing Pain Management
- 5 Signs You Are Enabling A Family Member’s Drug Addiction
- Drug Addiction And The Brain







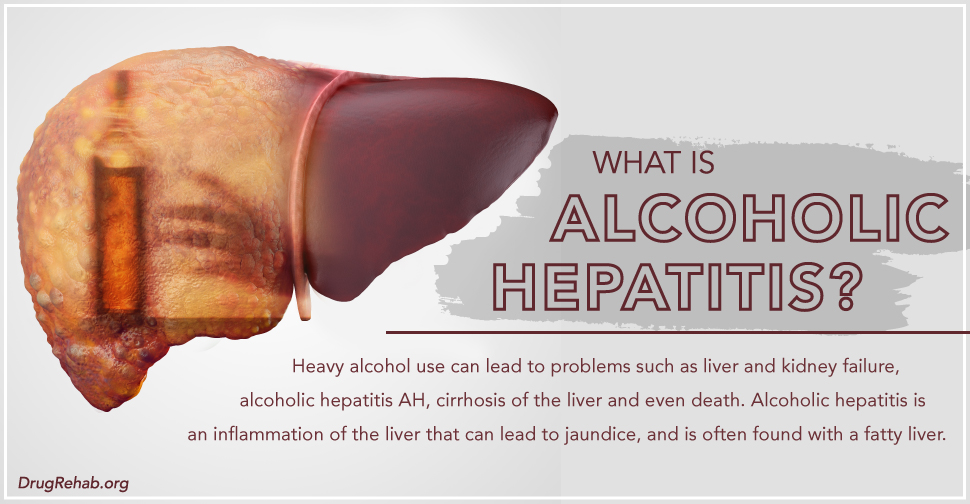





 If you think that someone might be too drunk, it’s important to keep an eye on them—a lot of people die in their sleep from alcohol poisoning. If your friend is unresponsive call 911, and try to turn them onto their side. Keep them sitting upright if they’re still awake, and get them to drink some water.
If you think that someone might be too drunk, it’s important to keep an eye on them—a lot of people die in their sleep from alcohol poisoning. If your friend is unresponsive call 911, and try to turn them onto their side. Keep them sitting upright if they’re still awake, and get them to drink some water.





 Fighting cancer can be a pretty scary business, and the pain it causes can be unbearable; someone who is suffering a terminal illness like cancer is likely to be in unimaginable pain. Pain is actually reported to be the biggest fear of someone suffering from cancer; not death, and not the loss of their life, but pain. For a person suffering with an often incurable condition, sometimes the only thing medical professionals can do is give them painkillers and anxiety medication to help them feel comfortable.
Fighting cancer can be a pretty scary business, and the pain it causes can be unbearable; someone who is suffering a terminal illness like cancer is likely to be in unimaginable pain. Pain is actually reported to be the biggest fear of someone suffering from cancer; not death, and not the loss of their life, but pain. For a person suffering with an often incurable condition, sometimes the only thing medical professionals can do is give them painkillers and anxiety medication to help them feel comfortable.
 The medical fraternity has come a long way in treating an addiction. Sometimes
The medical fraternity has come a long way in treating an addiction. Sometimes 

 Drug abuse has the potential to create numerous health effects, both physical and mental, within the lives of those who abuse. When a mental health disorder occurs with drug abuse, the two often worsen each other. Cocaine abuse, especially prolonged use, changes a person’s brain, affecting various chemical components, including certain important neurotransmitters which are critical within regulating a person’s mood. This effect may worsen existing depression or create new symptoms. Together, these disorders require effective substance abuse treatment.
Drug abuse has the potential to create numerous health effects, both physical and mental, within the lives of those who abuse. When a mental health disorder occurs with drug abuse, the two often worsen each other. Cocaine abuse, especially prolonged use, changes a person’s brain, affecting various chemical components, including certain important neurotransmitters which are critical within regulating a person’s mood. This effect may worsen existing depression or create new symptoms. Together, these disorders require effective substance abuse treatment. When using cocaine, there are several things which transpire concerning different aspects of the brain. Various neurotransmitters are affected, including the release of dopamine. When it comes to a sense of well-being, dopamine is the chemical which is considered to bring forth all kinds of pleasure and happy feelings. Dopamine releases when related to pleasure or a feeling of reward when it comes to specific activities in life. If dopamine levels become too high in the brain, they are linked to hallucinations, aggressiveness, delusions, anger, as well as other
When using cocaine, there are several things which transpire concerning different aspects of the brain. Various neurotransmitters are affected, including the release of dopamine. When it comes to a sense of well-being, dopamine is the chemical which is considered to bring forth all kinds of pleasure and happy feelings. Dopamine releases when related to pleasure or a feeling of reward when it comes to specific activities in life. If dopamine levels become too high in the brain, they are linked to hallucinations, aggressiveness, delusions, anger, as well as other  After extreme abuse over a period of time, stopping the use of cocaine can lead to cravings and depression for months. In some cases, suicidal thoughts may also occur. As someone faces withdrawal, the cravings grow more intense, even though the pleasurable effects of cocaine dip way down, instead becoming replaced by paranoia. When someone is facing withdrawal, here are some of the symptoms that may occur:
After extreme abuse over a period of time, stopping the use of cocaine can lead to cravings and depression for months. In some cases, suicidal thoughts may also occur. As someone faces withdrawal, the cravings grow more intense, even though the pleasurable effects of cocaine dip way down, instead becoming replaced by paranoia. When someone is facing withdrawal, here are some of the symptoms that may occur: Memories and information-processes are highly restricted when someone uses cocaine over the long term. “The reduced activity of the temporal lobe indicates that this structure is somehow compromised,” says Dr. Nancy Pilotte of NIDA’s Division of Basic Neuroscience and Behavioral Research. “Some of these regions mediate the ability to connect emotionally, and cocaine’s blunting of them may induce a flattened affect similar to depression symptoms that are common among chronic cocaine abusers.”
Memories and information-processes are highly restricted when someone uses cocaine over the long term. “The reduced activity of the temporal lobe indicates that this structure is somehow compromised,” says Dr. Nancy Pilotte of NIDA’s Division of Basic Neuroscience and Behavioral Research. “Some of these regions mediate the ability to connect emotionally, and cocaine’s blunting of them may induce a flattened affect similar to depression symptoms that are common among chronic cocaine abusers.”
 Every little kid walks through a dark alley and gets the heebie jeebies, it’s just part of growing up. As they get older and recognize that there is no boogie man there to get them, they relinquish the fear and grow out of it. Some people go through life with that constant fear that something bad will happen. They very well could be suffering from a panic attack, which is defined by the
Every little kid walks through a dark alley and gets the heebie jeebies, it’s just part of growing up. As they get older and recognize that there is no boogie man there to get them, they relinquish the fear and grow out of it. Some people go through life with that constant fear that something bad will happen. They very well could be suffering from a panic attack, which is defined by the  Not every substance will cause a panic attack, however, there are certain drugs that can. Some people suffering from a
Not every substance will cause a panic attack, however, there are certain drugs that can. Some people suffering from a  Caffeine is not always associated with substance abuse; however, it’s still a drug. When caffeine is consumed in heavy quantities, or more than a healthy amount, that’s abuse. Caffeine is a stimulant, and after it’s ingested (whether it’s in a pill form or in a beverage) it raises the heart rate. According to the
Caffeine is not always associated with substance abuse; however, it’s still a drug. When caffeine is consumed in heavy quantities, or more than a healthy amount, that’s abuse. Caffeine is a stimulant, and after it’s ingested (whether it’s in a pill form or in a beverage) it raises the heart rate. According to the  Alcohol is a drug which is sometimes referred to as “liquid courage”, because it can cause a person to do things that they might not normally do. Alcohol can lead to mood swings and temper tantrums–a person who abuses alcohol may exhibit bouts of rage, anxiety, and increased danger to his or herself and others. Withdrawal from alcohol can also lead to symptoms such as anxiety and panic attacks, but it can also lead to insomnia, delirium tremens, sweating profusely,
Alcohol is a drug which is sometimes referred to as “liquid courage”, because it can cause a person to do things that they might not normally do. Alcohol can lead to mood swings and temper tantrums–a person who abuses alcohol may exhibit bouts of rage, anxiety, and increased danger to his or herself and others. Withdrawal from alcohol can also lead to symptoms such as anxiety and panic attacks, but it can also lead to insomnia, delirium tremens, sweating profusely,  Marijuana can be smoked, consumed, or “dabbed”–the highest dose of tetrahydrocannabinol THC which can be abused. THC is the primary compound found in marijuana, and it can have serious affects on the mind of a person using it. Abuse of marijuana can lead to lack of motivation, mood swings, anxiety, and panic attacks. The
Marijuana can be smoked, consumed, or “dabbed”–the highest dose of tetrahydrocannabinol THC which can be abused. THC is the primary compound found in marijuana, and it can have serious affects on the mind of a person using it. Abuse of marijuana can lead to lack of motivation, mood swings, anxiety, and panic attacks. The 
 Opioids such as heroin are characterized by spurts of intense euphoria and well-being. Abusing drugs like heroin can lead to anxiety, severe depression, and insomnia. Even after a person stops using opioids, the withdrawals can start after a couple hours and last for several weeks–withdrawal symptoms can be incredibly dangerous and sometimes include paranoia, anxiety, panic, and seizures. With the prolonged withdrawals associated with opioids, relapse is more likely to occur to avoid further withdrawals.
Opioids such as heroin are characterized by spurts of intense euphoria and well-being. Abusing drugs like heroin can lead to anxiety, severe depression, and insomnia. Even after a person stops using opioids, the withdrawals can start after a couple hours and last for several weeks–withdrawal symptoms can be incredibly dangerous and sometimes include paranoia, anxiety, panic, and seizures. With the prolonged withdrawals associated with opioids, relapse is more likely to occur to avoid further withdrawals. Hallucinogens can give the user visual and mental delusions–or hallucinations. A person who is abusing hallucinogens (such as LSD, Peyote, PCP, and Psilocybin Mushrooms (or Shrooms)) can become dangerously antisocial. They might experience bouts of laughter, which can be followed by unexplainable crying. A person using these kind of drugs can very quickly slip into a drug induced panic attack, or lapse into paranoia. Withdrawal from some hallucinogens can be feeling of emptiness, prolonged trip (or “permi-trip”), inability to eat, anxiety, and fatigue.
Hallucinogens can give the user visual and mental delusions–or hallucinations. A person who is abusing hallucinogens (such as LSD, Peyote, PCP, and Psilocybin Mushrooms (or Shrooms)) can become dangerously antisocial. They might experience bouts of laughter, which can be followed by unexplainable crying. A person using these kind of drugs can very quickly slip into a drug induced panic attack, or lapse into paranoia. Withdrawal from some hallucinogens can be feeling of emptiness, prolonged trip (or “permi-trip”), inability to eat, anxiety, and fatigue.
 Despite its legal standing, prevalence, and acceptance within numerous social spheres, alcohol is not a benign drug. One of the most common and destructive ways in which this occurs is within circumstances regarding an individual driving after they have been drinking. In decades past, this behavior was more commonplace and even somewhat socially acceptable. Fortunately now, with the advent of more strident rules and social perspectives, this behavior has declined, as evidenced, in part, by statistics presented by the
Despite its legal standing, prevalence, and acceptance within numerous social spheres, alcohol is not a benign drug. One of the most common and destructive ways in which this occurs is within circumstances regarding an individual driving after they have been drinking. In decades past, this behavior was more commonplace and even somewhat socially acceptable. Fortunately now, with the advent of more strident rules and social perspectives, this behavior has declined, as evidenced, in part, by statistics presented by the 
 Yes. While you will likely be able to choose most any program, there are certain programs that are especially designed for DUI/DWI offenders. According to the Substance Abuse and Mental Health Services Administration (SAMHSA) “
Yes. While you will likely be able to choose most any program, there are certain programs that are especially designed for DUI/DWI offenders. According to the Substance Abuse and Mental Health Services Administration (SAMHSA) “
 Autism is much more common today than it was in past decades. The current number of children affected by autism is a ten-fold increase from forty years ago, according to Psychology Today. Research suggests autism gets its start in early brain development; one of the suggested ways to prevent autism for pregnant mothers is a diet high in folic acid. However, autism may be diagnosed in children two to three years of age—when symptoms tend to become obvious. Autism is also more common in boys than in girls.
Autism is much more common today than it was in past decades. The current number of children affected by autism is a ten-fold increase from forty years ago, according to Psychology Today. Research suggests autism gets its start in early brain development; one of the suggested ways to prevent autism for pregnant mothers is a diet high in folic acid. However, autism may be diagnosed in children two to three years of age—when symptoms tend to become obvious. Autism is also more common in boys than in girls. Autism is not typically associated with alcohol or drug abuse. Psychology Today explains that people with autism are traditionally not drawn to alcohol abuse because they tend to have a “preference for low risk and avoidance of social situations.” But the newest findings point to a heightened risk of addiction for those with autism. When two disorders occur together, they are called
Autism is not typically associated with alcohol or drug abuse. Psychology Today explains that people with autism are traditionally not drawn to alcohol abuse because they tend to have a “preference for low risk and avoidance of social situations.” But the newest findings point to a heightened risk of addiction for those with autism. When two disorders occur together, they are called  The goal for those with autism is often to move them into a manageable state of the disorder, and some reach this level. For those who don’t, and who develop addiction to drugs or alcohol, treatment is the best help available.
The goal for those with autism is often to move them into a manageable state of the disorder, and some reach this level. For those who don’t, and who develop addiction to drugs or alcohol, treatment is the best help available. 
 There are two different kinds of blood cells; white and red. White blood cells are essential for a body’s resistance to infection, and red blood cells are vital for energy and transporting oxygen. It is the bone marrow which is responsible for creating white and red blood cells. Alcohol abuse interferes with the bone marrows abilities to produce those cells, leaving a person tired, weak, and vulnerable to infection.
There are two different kinds of blood cells; white and red. White blood cells are essential for a body’s resistance to infection, and red blood cells are vital for energy and transporting oxygen. It is the bone marrow which is responsible for creating white and red blood cells. Alcohol abuse interferes with the bone marrows abilities to produce those cells, leaving a person tired, weak, and vulnerable to infection. Bone marrow suppression from heavy alcohol abuse can be linked to various diseases such as: Myelodysplastic Syndrome- which is characterized by mutated cells, Paroxysmal nocturnal hemoglobinuria- or blood in the urine and is fatal to
Bone marrow suppression from heavy alcohol abuse can be linked to various diseases such as: Myelodysplastic Syndrome- which is characterized by mutated cells, Paroxysmal nocturnal hemoglobinuria- or blood in the urine and is fatal to  So what do we know about Alcohol Abuse? A person who abuses alcohol might drink alcohol daily and completely lose control each time, or only get drunk on the weekend. It doesn’t make a difference, they are both forms of alcohol abuse.
So what do we know about Alcohol Abuse? A person who abuses alcohol might drink alcohol daily and completely lose control each time, or only get drunk on the weekend. It doesn’t make a difference, they are both forms of alcohol abuse.

 This program is perhaps one of the better-known support groups for people recovering from substance abuse. It is open to people who are victims of any substance abuse. The 12 steps of the program help guide participants through recovery by asking them to uphold principles. Some of these include committing to a healthy lifestyle, putting faith in a higher power (defined at will), and engaging in self-love and self-awareness.
This program is perhaps one of the better-known support groups for people recovering from substance abuse. It is open to people who are victims of any substance abuse. The 12 steps of the program help guide participants through recovery by asking them to uphold principles. Some of these include committing to a healthy lifestyle, putting faith in a higher power (defined at will), and engaging in self-love and self-awareness. Pills Anonymous is a support group dedicated to members who want recovery from prescription drug (pills) abuse. As described on the organization’s web page, this program, “is a fellowship of men and women who share their experience strength and hope with each other that they may solve their common problem and help others to recover from pill addiction.” The group does not have any ties to religions, political parties, etc. Members attend meetings, participate in a 12-step program, and work to help others achieve long-term recovery success.
Pills Anonymous is a support group dedicated to members who want recovery from prescription drug (pills) abuse. As described on the organization’s web page, this program, “is a fellowship of men and women who share their experience strength and hope with each other that they may solve their common problem and help others to recover from pill addiction.” The group does not have any ties to religions, political parties, etc. Members attend meetings, participate in a 12-step program, and work to help others achieve long-term recovery success. 4-point program adapted from a scientific approach. The four points include:
4-point program adapted from a scientific approach. The four points include:





 Agitation
Agitation
 One of the biggest changes between the DSM-IV and DSM-V criteria, is the
One of the biggest changes between the DSM-IV and DSM-V criteria, is the 
