
Ambien (generic name zolpidem) is a medication used to treat insomnia. A sedative hypnotic, it works due to the way it reduces brain activity. Used properly, Ambien is typically safe. However, when misused, it does hold potential for abuse. Misusing your prescription or using this drug recreationally could lead to addiction. Ambien abuse is dangerous, with adverse effects ranging from withdrawal, memory loss, organ damage, overdose, and more.
Ambien was originally thought to be safer than benzodiazepines, a class of drugs commonly prescribed for sleep disorders. In line with this thinking, prescriptions for this drug climbed. Subsequently, the opportunity for misuse and drug diversion rose as well. Contrary to these beliefs, over time, widespread reports of abuse and addiction surfaced. In July of 2002, zolpidem was classified as Schedule IV, the same category as benzodiazepine drugs.
What Is Ambien?
Ambien is a “Z-drug,” or nonbenzodiazepine drug. Despite this, its mechanism of action is actually similar to that of benzodiazepine sleeping aids. This is due to the way it binds to GABA-A receptors at benzodiazepine binding sites within the brain, as explained by the British Journal of Clinical Pharmacology (BJCP). It should be taken directly before sleeping and only if you’re confident you’ll be able to stay in bed for seven to eight hours.
Ambien comes in a tablet form, either as an immediate release tablet or as the controlled-release version (Ambien CR). This medication only be used for short periods of time. This is due to the fact that after two weeks the efficacy may decline. Also, after more prolonged use the risk of dependence and withdrawal climbs.
Is Ambien Addictive?
The Journal of Research in Medical Sciences writes that “zolpidem can exert abuse capability, euphoric mood, tolerance, and withdrawal syndrome,” all of which increase a person’s risk for addiction. Typically, if you use Ambien as prescribed, the drug has a limited potential for dependence and abuse. The problem arises if you begin to misuse your medication, even if you’re simply seeking to self-medicate insomnia. This is considered abuse.
Recreational users may take the drug orally or snort it and often force themselves to stay awake so that they can experience the “feel good” effects. People abuse this drug to achieve a sedated and euphoric state similar to drunkenness. Some users claim they take it to increase pleasurable feelings during sex.
Over time, these individuals may need to take more of the drug to create this effect (a tolerance). Using Ambien in these ways puts a person at a greater risk for addiction. Individuals with a history of substance abuse or a mental illness face a heightened risk for Ambien abuse and addiction.
What Are The Side Effects And Symptoms Of Ambien Abuse?
According to the FDA , prescribed Ambien use can cause abnormal thinking, behavioral changes, complex behaviors, hallucinations, thoughts of suicide, or worsening depression. Ambien abuse could intensify these adverse effects and may also cause:

- Agitation
- Aggression
- Becoming more outgoing
- Bizarre behaviors
- Confusion
- Daytime drowsiness
- Decreased inhibitions
- Delirium
- Dizziness
- Dry mouth
- Gastrointestinal troubles
- Headache
- Impaired coordination
- Impaired judgement
- Memory lapses, amnesia, or blackouts
- Nightmares
- Shallow or slowed breathing
- Sleepwalking
- Slowed reflexes
- Slurred speech
Tolerance and withdrawal are signs of abuse, though they can occur with prescribed use as well. Within addiction, these factors are accompanied by compulsive and chronic drug-seeking.
What Are The Dangers Of Ambien Abuse And Addiction?
Ambien is a central nervous system (CNS) depressant. This means it slows down your heart and breathing rates. Because of this, using it with alcohol or other CNS depressants like benzos or opioid painkillers may be dangerous. According to a 2014 DAWN Report, from 2005 to 2010 “the number of zolpidem-related emergency department (ED) visits involving adverse reactions increased nearly 220 percent.” In 2010, women made up two thirds of these visits, while 50 percent involved other medications.
Ambien has been linked to an increased risk of:
- Addiction
- Anxiety
- Depression
- Falls and injury
- Psychosis
- Risky sexual behaviors
- Stroke
- Suicide
- Violence
- Withdrawal seizures
- Other diseases and illness
The FDA cautions that driving the morning after taking Ambien could be dangerous, due to the drug’s intensely sedative effects. This is especially true with the CR version.
A BMJ Open article asserted that individuals taking sleeping pills, including zolpidem faced a four times greater risk of death and for those taking larger doses, a 35 percent higher risk of cancer. Others studies find that zolpidem is associated with a seven times higher risk of acute pancreatitis and within elderly users, reversible dementia.
The Daily Express outlined a study which found an increased risk of heart attack and life-threatening cardiac events. The news source reported that “four standard dose pills a year – 35 milligrams – send the risk soaring by around 20 per cent. People taking the equivalent of 60 tablets a year could see the threat jump by half.”
Ambien Can Be Dangerous Even While You Sleep
Even within the bounds of prescribed use an individual may experience “complex sleep-related behaviors,” including operating a vehicle, cooking or eating while sleeping, or having sleep sex. These circumstances may be very dangerous and have been reported to cause car accidents, kitchen fires, consumption of toxic chemicals, and unintended pregnancies.
A Huffington Post article chronicled bizarre and catastrophic behavior which occurred under the influence of Ambien. The most frightening circumstance included a man murdering eight people. Others included sleep driving episodes which resulted in great bodily harm to pedestrians (death could also occur). Shocking accounts of Ambien being used as a date rape drug were also detailed. Abusing larger dosages of Ambien could increase the risk of these and other complex sleep-related behaviors.
Can You Overdose From Ambien?
Like many other drugs of abuse, Ambien does have the potential to cause overdose when taken in higher dosages. This danger spikes with polydrug abuse. Women and older individuals eliminate the drug more slowly which can also heighten the risk. Signs of overdose include:
- Extreme drowsiness
- Decreased heartbeat
- Slowed breathing
- Losing consciousness
- Seizure
- Coma
Overdose can be life threatening. Should you suspect that yourself or someone else is at risk, contact emergency medical staff immediately.
How Is Ambien Addiction Treated?
Ambien abuse and addiction should be taken seriously. In more mild instances, outpatient treatment may be sufficient. For those who suffer from more serious cases or polydrug addiction, inpatient drug rehab is recommended. As this drug can create uncomfortable symptoms of withdrawal, it should be slowly tapered. A medically supervised detox may be advised and may include the use of certain non-addictive medications to alleviate withdrawal symptoms.
Addiction often results from a person self-medicating mental or emotional trouble. Effective rehab programs use behavioral therapy and counseling to address these concerns. These may be enhanced by treatment for co-occurring disorders, family therapy and support, and peer support groups. If you or a loved one stumbled into Ambien addiction by misusing the drug to self-medicate insomnia, treatment may help. Your recovery plan may include addressing this issue in an alternative way.
Get Help Today
If you’re fearful that your Ambien use is accelerating into abuse or addiction, reach out today. Together, we can build a plan to get your life back on track. DrugRehab.org is here to help you find and experience the freedom of sobriety. Contact us now.
For More Information Related to “Ambien Addiction And Treatment Options” Be Sure To Check Out These Additional Resources From DrugRehab.org:
- Consequences Of Injecting OxyContin (Oxycodone)
- Klonopin Withdrawal Symptoms
- How To Treat Vyvanse Addiction
- The Dangers Of Snorting Vicodin (Hydrocodone)
- Environmental Risk Factors for Developing an Addiction
- Drug Addiction And The Brain
Sources
MedlinePlus — Zolpidem
SpringerLink — Increased relative risk of acute pancreatitis in zolpidem users
U.S. Food and Drug Administration — Highlights of Prescribing Information
U.S. National Library of Medicine — An Increased Risk of Reversible Dementia May Occur After Zolpidem Derivative Use in the Elderly Population
U.S. National Library of Medicine — Prescription Sedative Misuse and Abuse









 Prescription sedatives are used in medicine to help a person more comfortably deal with insomnia, anxiety, epilepsy, pain, hyperactive disorders, attention disorders, and other mental disorders. Even if a person is using the recommended dosage of a prescribed sedative, they may be at a great risk of becoming addicted. Misuse of sedatives is usually a result of euphoria that it brings them, but abusing drugs can lead to trouble. According to the
Prescription sedatives are used in medicine to help a person more comfortably deal with insomnia, anxiety, epilepsy, pain, hyperactive disorders, attention disorders, and other mental disorders. Even if a person is using the recommended dosage of a prescribed sedative, they may be at a great risk of becoming addicted. Misuse of sedatives is usually a result of euphoria that it brings them, but abusing drugs can lead to trouble. According to the  Xanax( or Alprazolam) is used for treating anxiety and panic disorders, it is effective in slowing down abnormal brain activity. It can also be used for depression, agoraphobia, and premenstrual symptoms. Xanax can be a habit forming drug, especially when it is taken in larger than the suggested dose, or when dosage is continued further than what is suggested by a doctor. When a person stops using Xanax they might experience withdrawals and symptoms like irritability, aggressiveness, diarrhea, decrease in appetite, weight loss, shakiness, and seizures.
Xanax( or Alprazolam) is used for treating anxiety and panic disorders, it is effective in slowing down abnormal brain activity. It can also be used for depression, agoraphobia, and premenstrual symptoms. Xanax can be a habit forming drug, especially when it is taken in larger than the suggested dose, or when dosage is continued further than what is suggested by a doctor. When a person stops using Xanax they might experience withdrawals and symptoms like irritability, aggressiveness, diarrhea, decrease in appetite, weight loss, shakiness, and seizures. Valium (or Diazapam) is used used for treatment of anxiety, seizures, muscle spasms, and can also be used to treat a patient who is experiencing alcohol withdrawals. A person who abuses Valium will likely build up a tolerance to the drug, and can become dependent on it. A person who is dependent on the drug Valium can experience terrible withdrawal symptoms when the drug is no longer available. Withdrawals can consist of worsening conditions and lead to panic attacks, insomnia, and aggressiveness.
Valium (or Diazapam) is used used for treatment of anxiety, seizures, muscle spasms, and can also be used to treat a patient who is experiencing alcohol withdrawals. A person who abuses Valium will likely build up a tolerance to the drug, and can become dependent on it. A person who is dependent on the drug Valium can experience terrible withdrawal symptoms when the drug is no longer available. Withdrawals can consist of worsening conditions and lead to panic attacks, insomnia, and aggressiveness. Ambien (Zolpidem) is used to slow down brain activity to help a person sleep. A person should not take Ambien for longer than two weeks, because it can also be habit forming. Some people abuse Ambien, by taking large doses or using the drug for something other than treating a medical condition. Ambien and other sedatives like it can cause hallucination-like feelings for person abusing the drug.
Ambien (Zolpidem) is used to slow down brain activity to help a person sleep. A person should not take Ambien for longer than two weeks, because it can also be habit forming. Some people abuse Ambien, by taking large doses or using the drug for something other than treating a medical condition. Ambien and other sedatives like it can cause hallucination-like feelings for person abusing the drug.
 Also known as Lorazepam, Ativan is prescribed to treat anxiety; but can also be used for epilepsy and irritable bowel syndrome. It slows the brain to help a person relax, but if an excessive amount of Ativan is taken, a person can overdose. Ativan is habit forming if taken longer than prescribed or if taken in larger doses than suggested.
Also known as Lorazepam, Ativan is prescribed to treat anxiety; but can also be used for epilepsy and irritable bowel syndrome. It slows the brain to help a person relax, but if an excessive amount of Ativan is taken, a person can overdose. Ativan is habit forming if taken longer than prescribed or if taken in larger doses than suggested. Lunesta is used to treat insomnia, and is categorized under the drug hypnotics–a person who abuses Lunesta may do so because it slows down the brain function. A user may experience hallucinations if they do not go to sleep shortly after taking Lunesta. Overdose is likely to occur if a person takes more than the recommended dose, and after a person stops taking Lunesta, they can experience withdrawals and have trouble sleeping.
Lunesta is used to treat insomnia, and is categorized under the drug hypnotics–a person who abuses Lunesta may do so because it slows down the brain function. A user may experience hallucinations if they do not go to sleep shortly after taking Lunesta. Overdose is likely to occur if a person takes more than the recommended dose, and after a person stops taking Lunesta, they can experience withdrawals and have trouble sleeping.
 For those that are struggling with an opiate addiction and are either not able to find or afford their drug of choice or are struggling with the symptoms of withdrawal as they attempt to stop using it, taking loperamide seems like a simple way to obtain their goals.
For those that are struggling with an opiate addiction and are either not able to find or afford their drug of choice or are struggling with the symptoms of withdrawal as they attempt to stop using it, taking loperamide seems like a simple way to obtain their goals. Though the effect is minimal, and not encountered by every person that takes this drug in large proportions, some people take massive doses for recreational purposes and claim that they experience a more minimal sense of the high or euphoria that other opiates create.
Though the effect is minimal, and not encountered by every person that takes this drug in large proportions, some people take massive doses for recreational purposes and claim that they experience a more minimal sense of the high or euphoria that other opiates create.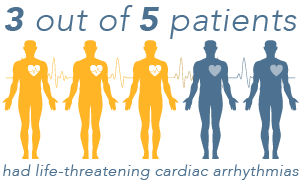 The study’s authors spoke of two individuals that took massive quantities of loperamide and subsequently overdosed. Emergency services were contacted and what followed for both failed to prove life-saving. Despite medical intervention and support, including “manual cardiopulmonary resuscitation (CPR),
The study’s authors spoke of two individuals that took massive quantities of loperamide and subsequently overdosed. Emergency services were contacted and what followed for both failed to prove life-saving. Despite medical intervention and support, including “manual cardiopulmonary resuscitation (CPR), 





 In fact, another study in 2013 (performed at the Indiana University Center For Aging Research) had already found many of the same effects in anticholinergic drugs. They found that the drugs caused serious cognitive problems and could occur as quickly as 60 days after the first dose. The problem with replacing these drugs is that many people (especially the elderly) rely on them to stay healthy. As a result, cognitive impairment and even an increased risk of dementia have been noted in people who continue to use them. This finding could potentially have a wide impact on the medical market and may require doctors and patients find alternative treatments for the many medical uses of anticholinergic drugs.
In fact, another study in 2013 (performed at the Indiana University Center For Aging Research) had already found many of the same effects in anticholinergic drugs. They found that the drugs caused serious cognitive problems and could occur as quickly as 60 days after the first dose. The problem with replacing these drugs is that many people (especially the elderly) rely on them to stay healthy. As a result, cognitive impairment and even an increased risk of dementia have been noted in people who continue to use them. This finding could potentially have a wide impact on the medical market and may require doctors and patients find alternative treatments for the many medical uses of anticholinergic drugs.





