
Mixing a benzodiazepine like Xanax with an opioid like oxycodone can increase the chance of respiratory depression, slowed breathing, slowed heart rate, overdose, and death. Benzodiazepines and opioids are highly addictive substances that can be difficult, and dangerous, to stop using alone. Professional treatment can help someone quit by teaching them to replace unhealthy habits and behaviors with healthy ones.
Understanding Xanax And Oxycodone Abuse
Xanax is the most popular brand name of alprazolam and belongs to a class of medications known as benzodiazepines. Benzodiazepines (benzos) are a type of sedative most commonly used to treat anxiety disorders and panic disorders. Xanax works by slowing down a person’s central nervous system and helping them feel relaxed.
Opioids like oxycodone are also known to slow down the central nervous system (CNS), and are commonly used in medicine to relieve moderate to severe pain. Oxycodone is the generic version of OxyContin. Because of the potency of oxycodone, physicians will regulate the amount of the drug that’s prescribed.

The problem is that both benzodiazepines and opioids often elicit a feeling of well-being and euphoria. It’s because of that feeling that people abuse each medication to get “high.” Opioids can make a person feel numb, drowsy, and elated. Mixing opioids with benzodiazepines causes that high to be intensified. This can be a dangerous combination, even with a small amount of each drug.
You may be wondering, “if these drugs are so dangerous, then how and why are people getting them?” Oftentimes, after a person starts abusing prescription medications, they start doctor shopping, and lying about symptoms. It can be very difficult for a physician to tell who’s telling the truth and who isn’t.
The predicament is actually getting worse. “The number of patients prescribed both an opioid pain reliever and a benzodiazepine increased by 41 percent between 2002 and 2014. That translates to an increase of more than 2.5 million opioid painkiller patients also receiving benzodiazepines,”(CBS News).
What Are The Consequences Of Prescription Drug Abuse?
Mixing opioids and benzodiazepines is incredibly dangerous, so much that the Food and Drug Administration (FDA) has cautioned physicians and patients about mixing the two. The FDA stated, that “healthcare professionals should limit prescribing opioid pain medicines with benzodiazepines or other CNS depressants only to patients for whom alternative treatment options are inadequate.”
The FDA went on to say that “patients taking opioids with benzodiazepines, other CNS depressant medicines, or alcohol, and caregivers of these patients, should seek medical attention immediately if they or someone they are caring for experiences symptoms of unusual dizziness or lightheadedness, extreme sleepiness, slowed or difficult breathing, or unresponsiveness.”
In other words, mixing benzodiazepines and opioids increases this risk of overdose, and death. In 2015, there were 6,872 overdose deaths from benzodiazepines, and 5,826 of those deaths involved opioids.
Not only can abusing prescription drugs result in overdose, it can cause a mental addiction, or physical dependence as well. Mixing benzos and opioids can also lead to serious health problems with the liver, heart, brain, and stomach.
Opioids can be dangerous without the help of Xanax, and according to the Center for Disease Control and Prevention, “opioids killed more than 33,000 people in 2015, more than any year on record. Nearly half of all opioid overdose deaths involve a prescription opioid.”
What Are The Symptoms Of Withdrawal?
Whether they’re taken for a legitimate medical purpose or not, prescription Xanax and oxycodone can lead to a physical dependency. This essentially means that when a person stops taking the drugs, their body continues craving the active chemical.
Because opioids and benzodiazepines are both mentally and physically addictive, most people will experience physical and mental withdrawal symptoms when they stop. When opioids and benzos are mixed, the results are often unpredictable.

When a person quits using oxycodone, they may experience withdrawal that has potential to cause them to relapse. These withdrawal symptoms, according to the U.S. National Library of Medicine, may include:
- restlessness
- watery eyes
- runny nose
- sneezing
- yawning
- sweating
- chills
- muscle or joint aches or pains
- weakness
- irritability
- anxiety
- depression
- difficulty falling asleep or staying asleep
- cramps
- nausea
- vomiting
- diarrhea
- loss of appetite
- fast heartbeat
- fast breathing
Stopping benzodiazepines cold-turkey can be very dangerous as well, and often intensifies withdrawal. It is for this reason that a physician will gradually decrease dosage. The withdrawal symptoms of Xanax, according to NLM, may include:
- seizures
- headache
- blurred vision
- increased sensitivity to noise or light
- change in sense of smell
- sweating
- difficulty falling asleep or staying asleep
- difficulty concentrating
- nervousness
- depression
- irritability
- aggressive behavior
- muscle twitching or cramps
- diarrhea
- vomiting
- pain
- burning
- numbness
- or tingling in the hands or feet
- a decrease in appetite
- weight loss
A medical detoxification can help a person safely remove a drug from their system while managing the symptoms of withdrawal. Detoxification may be required to properly treat an addiction to both benzodiazepines and opioids.
How Do People Become Addicted To Prescription Drugs?
Even when a person takes Xanax or oxycodone as a prescription, they’re at risk of becoming addicted to them. What usually happens with oxycodone, is someone starts out with an injury that requires pain relief. They take the medicine with no intention to abuse it, but overtime, with continued use, they begin to build up a tolerance and then become dependent.
At this point, they might enjoy the feeling oxycodone gives them. Many people who become dependent on opioids continue taking the drug just to avoid relapse, and might even switch to street drugs like heroin, because it can be less expensive while creating a more intense euphoria.
 This is only a potential scenario, and doesn’t apply to everyone—the point is that though not everyone abuses prescription drugs for the same reason, all of our minds are wired the same way to crave things that make us feel good.
This is only a potential scenario, and doesn’t apply to everyone—the point is that though not everyone abuses prescription drugs for the same reason, all of our minds are wired the same way to crave things that make us feel good.
It can be really hard to understand why prescription medicines are so dangerous, but still used. The fact is that some people suffer from serious mental disorders while others have severe pain. These types of people still need medicine to help them deal with their illnesses or conditions.
NIDA for Teens described how addiction works, by stating that “prescription drugs that effect the brain, including opioid pain relievers, stimulants, and depressants, can cause physical dependence that could lead to addiction.
Medications that affect the brain can change the way it works—especially when they are taken over an extended period of time or with escalating doses. They can change the reward system, making it harder for a person to feel good without the drug and possibly leading to intense cravings, which make it hard to stop using.”
There are other factors that can play a part in addiction as well. These may include environmental, biological, or psychological variables. Some people suffer from mental disorders that require a medication like Xanax. This can be a difficult situation, because as a they continue using Xanax, they’re at a greater risk of becoming dependent, but if they stop using the drug they’re mental condition could worsen—this is where millions are met with a dilemma.
Not everyone’s addiction is the same either, so treating the addiction will be different for each person as well. There are behavioral and physical symptoms that usually need to be tended to in order for a treatment to be successful.
At the end of the day, addiction to benzodiazepines and opioids is not easy to overcome, but it’s still possible. Some of the different treatment programs that can help along the path to recovery include:
- Medical Detoxification
- Medication-Assisted Therapy
- Cognitive Behavioral Therapy
- Dialectical Behavioral Therapy
- Inpatient or Outpatient Treatment
- Motivational Interviewing
- Mindfulness and Stress Management
Find Treatment For Substance Use Disorder And Addiction
If you or someone you love is struggling with prescription drugs, please don’t wait to reach out to us. Contact an addiction specialist at DrugRehab.org today to learn how to overcome addiction and build a solid foundation to lifelong recovery.
For More Information Related to “The Dangers of Mixing Xanax and Oxycodone” Be Sure To Check Out These Additional Resources From DrugRehab.org:
- Heroin and Opioid Addiction Statistics
- The Dangers of Snorting Oxycontin (Oxycodone)
- The Most Addictive Prescription Sedatives
- Serax (Oxazepam) Withdrawal and Detoxification
- Klonopin Withdrawal Symptoms
Sources
Center for Disease Control and Prevention – Opioid Overdose
National Institute on Drug Abuse – Overdose Death Rates
U.S. National Library of Medicine NLM – Alprazolam
U.S. National Library of Medicine NLM – Oxycodone



 Ativan is a brand name medication of the benzodiazepine (benzo) drug lorazepam. As a benzo, it’s a central nervous system (CNS) depressant, which means it slows several important bodily functions, including breathing rates, heart rate, and temperature. The
Ativan is a brand name medication of the benzodiazepine (benzo) drug lorazepam. As a benzo, it’s a central nervous system (CNS) depressant, which means it slows several important bodily functions, including breathing rates, heart rate, and temperature. The 
 Detox can be emotionally strenuous as well, which is another reason detoxing in a facility is so important. The facility’s staff will comfort you during this time, answering any questions you may have, or will simply provide an ear and any emotional support you may need.
Detox can be emotionally strenuous as well, which is another reason detoxing in a facility is so important. The facility’s staff will comfort you during this time, answering any questions you may have, or will simply provide an ear and any emotional support you may need.
 Temazepam is one of the many sedatives that can be used to help a person sleep, but in the illicit market, there’s a lot of room for diversion and abuse of it. Perhaps you’ve never heard of it, but temazepam a much bigger problem than most of us realize.
Temazepam is one of the many sedatives that can be used to help a person sleep, but in the illicit market, there’s a lot of room for diversion and abuse of it. Perhaps you’ve never heard of it, but temazepam a much bigger problem than most of us realize. Temazepam and other benzodiazepines are classified as schedule IV depressants by the
Temazepam and other benzodiazepines are classified as schedule IV depressants by the  During this time, you’ll gradually be taken off the benzodiazepine, and your withdrawal symptoms will be carefully monitored by professionals.
During this time, you’ll gradually be taken off the benzodiazepine, and your withdrawal symptoms will be carefully monitored by professionals.

 The FDA sums it up perfectly, “abuse is characterized by misuse of the drug for nonmedical purposes, often in combination with other psychoactive substances. Physical dependence is a state of adaptation that is manifested by a specific withdrawal syndrome that can be produced by abrupt cessation, rapid dose reduction, decreasing blood level of the drug and/or administration of an antagonist…Tolerance is a state of adaptation in which exposure to a drug induces changes that result in a diminution of one or more of the drug’s effects over time.”
The FDA sums it up perfectly, “abuse is characterized by misuse of the drug for nonmedical purposes, often in combination with other psychoactive substances. Physical dependence is a state of adaptation that is manifested by a specific withdrawal syndrome that can be produced by abrupt cessation, rapid dose reduction, decreasing blood level of the drug and/or administration of an antagonist…Tolerance is a state of adaptation in which exposure to a drug induces changes that result in a diminution of one or more of the drug’s effects over time.”












 Persistent drowsiness
Persistent drowsiness


 Prescription sedatives are used in medicine to help a person more comfortably deal with insomnia, anxiety, epilepsy, pain, hyperactive disorders, attention disorders, and other mental disorders. Even if a person is using the recommended dosage of a prescribed sedative, they may be at a great risk of becoming addicted. Misuse of sedatives is usually a result of euphoria that it brings them, but abusing drugs can lead to trouble. According to the
Prescription sedatives are used in medicine to help a person more comfortably deal with insomnia, anxiety, epilepsy, pain, hyperactive disorders, attention disorders, and other mental disorders. Even if a person is using the recommended dosage of a prescribed sedative, they may be at a great risk of becoming addicted. Misuse of sedatives is usually a result of euphoria that it brings them, but abusing drugs can lead to trouble. According to the  Xanax( or Alprazolam) is used for treating anxiety and panic disorders, it is effective in slowing down abnormal brain activity. It can also be used for depression, agoraphobia, and premenstrual symptoms. Xanax can be a habit forming drug, especially when it is taken in larger than the suggested dose, or when dosage is continued further than what is suggested by a doctor. When a person stops using Xanax they might experience withdrawals and symptoms like irritability, aggressiveness, diarrhea, decrease in appetite, weight loss, shakiness, and seizures.
Xanax( or Alprazolam) is used for treating anxiety and panic disorders, it is effective in slowing down abnormal brain activity. It can also be used for depression, agoraphobia, and premenstrual symptoms. Xanax can be a habit forming drug, especially when it is taken in larger than the suggested dose, or when dosage is continued further than what is suggested by a doctor. When a person stops using Xanax they might experience withdrawals and symptoms like irritability, aggressiveness, diarrhea, decrease in appetite, weight loss, shakiness, and seizures. Valium (or Diazapam) is used used for treatment of anxiety, seizures, muscle spasms, and can also be used to treat a patient who is experiencing alcohol withdrawals. A person who abuses Valium will likely build up a tolerance to the drug, and can become dependent on it. A person who is dependent on the drug Valium can experience terrible withdrawal symptoms when the drug is no longer available. Withdrawals can consist of worsening conditions and lead to panic attacks, insomnia, and aggressiveness.
Valium (or Diazapam) is used used for treatment of anxiety, seizures, muscle spasms, and can also be used to treat a patient who is experiencing alcohol withdrawals. A person who abuses Valium will likely build up a tolerance to the drug, and can become dependent on it. A person who is dependent on the drug Valium can experience terrible withdrawal symptoms when the drug is no longer available. Withdrawals can consist of worsening conditions and lead to panic attacks, insomnia, and aggressiveness. Ambien (Zolpidem) is used to slow down brain activity to help a person sleep. A person should not take Ambien for longer than two weeks, because it can also be habit forming. Some people abuse Ambien, by taking large doses or using the drug for something other than treating a medical condition. Ambien and other sedatives like it can cause hallucination-like feelings for person abusing the drug.
Ambien (Zolpidem) is used to slow down brain activity to help a person sleep. A person should not take Ambien for longer than two weeks, because it can also be habit forming. Some people abuse Ambien, by taking large doses or using the drug for something other than treating a medical condition. Ambien and other sedatives like it can cause hallucination-like feelings for person abusing the drug.
 Also known as Lorazepam, Ativan is prescribed to treat anxiety; but can also be used for epilepsy and irritable bowel syndrome. It slows the brain to help a person relax, but if an excessive amount of Ativan is taken, a person can overdose. Ativan is habit forming if taken longer than prescribed or if taken in larger doses than suggested.
Also known as Lorazepam, Ativan is prescribed to treat anxiety; but can also be used for epilepsy and irritable bowel syndrome. It slows the brain to help a person relax, but if an excessive amount of Ativan is taken, a person can overdose. Ativan is habit forming if taken longer than prescribed or if taken in larger doses than suggested. Lunesta is used to treat insomnia, and is categorized under the drug hypnotics–a person who abuses Lunesta may do so because it slows down the brain function. A user may experience hallucinations if they do not go to sleep shortly after taking Lunesta. Overdose is likely to occur if a person takes more than the recommended dose, and after a person stops taking Lunesta, they can experience withdrawals and have trouble sleeping.
Lunesta is used to treat insomnia, and is categorized under the drug hypnotics–a person who abuses Lunesta may do so because it slows down the brain function. A user may experience hallucinations if they do not go to sleep shortly after taking Lunesta. Overdose is likely to occur if a person takes more than the recommended dose, and after a person stops taking Lunesta, they can experience withdrawals and have trouble sleeping.




 Muscle relaxant
Muscle relaxant
 Avoiding drugs and situations that lead to drug use
Avoiding drugs and situations that lead to drug use
 With so many facing anxiety, stress, panic attacks, and seizures, benzodiazepines—such as diazepam (Valium) and alprazolam (Xanax)—are commonly being prescribed. There are 15 or more different types of benzodiazepine medications that treat a variety of medical issues. The multiplicity of benzodiazepines are used for: anxiety, muscle relaxant, amnesiac (mild-memory loss), and anticonvulsant. The less intense benzodiazepines, such as triazolam (Halcion) and estazolam (ProSom), are recommended for short-term treatment of sleep disorders. Usually, benzodiazepines are not prescribed for long-term use because of the risk of developing addiction.
With so many facing anxiety, stress, panic attacks, and seizures, benzodiazepines—such as diazepam (Valium) and alprazolam (Xanax)—are commonly being prescribed. There are 15 or more different types of benzodiazepine medications that treat a variety of medical issues. The multiplicity of benzodiazepines are used for: anxiety, muscle relaxant, amnesiac (mild-memory loss), and anticonvulsant. The less intense benzodiazepines, such as triazolam (Halcion) and estazolam (ProSom), are recommended for short-term treatment of sleep disorders. Usually, benzodiazepines are not prescribed for long-term use because of the risk of developing addiction. “This was a nail-in-the-coffin study to show that activity of dopaminergic neurons leads to synaptic adaptation that is involved in addiction,” said Dr. Lüscher. “This is why addiction is so difficult to treat. Even if you clear the drug from the body, there are long-lasting changes in
“This was a nail-in-the-coffin study to show that activity of dopaminergic neurons leads to synaptic adaptation that is involved in addiction,” said Dr. Lüscher. “This is why addiction is so difficult to treat. Even if you clear the drug from the body, there are long-lasting changes in 

 When used properly, Xanax (alprazolam) holds the potential to be a valuable tool in fighting generalized anxiety and other more extreme panic disorders, by helping people to combat their stress and maintain emotional and mental stability in their life. Xanax works towards depressing your central nervous system in a way that creates a calming state and the characteristic signs of sedation.
When used properly, Xanax (alprazolam) holds the potential to be a valuable tool in fighting generalized anxiety and other more extreme panic disorders, by helping people to combat their stress and maintain emotional and mental stability in their life. Xanax works towards depressing your central nervous system in a way that creates a calming state and the characteristic signs of sedation. Xanax is available in an extended-release version. What this means is that the pill is meant to be taken in its whole form, due to the fact that it is designed in a manner that gradually releases the medicine into your body. Sometimes when a person is abusing Xanax, they will alter the pill, either crushing it or breaking it apart. This affects the drug’s absorption, allowing it to be assimilated into your body quicker, creating a higher risk of overdose.
Xanax is available in an extended-release version. What this means is that the pill is meant to be taken in its whole form, due to the fact that it is designed in a manner that gradually releases the medicine into your body. Sometimes when a person is abusing Xanax, they will alter the pill, either crushing it or breaking it apart. This affects the drug’s absorption, allowing it to be assimilated into your body quicker, creating a higher risk of overdose.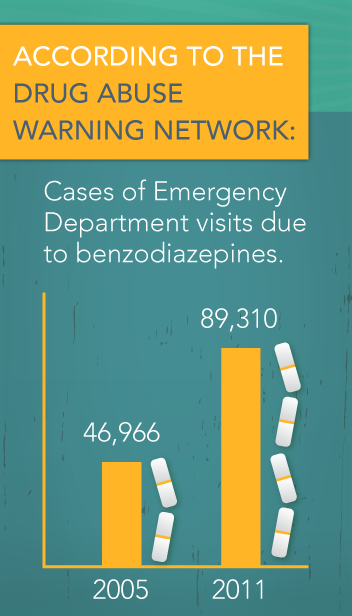 According to the Drug Abuse Warning Network, cases of Emergency Department visits due to benzodiazepines alone rose from 46,966 in 2005, to 89,310 in 2011, which is just over a 50 percent increase.
According to the Drug Abuse Warning Network, cases of Emergency Department visits due to benzodiazepines alone rose from 46,966 in 2005, to 89,310 in 2011, which is just over a 50 percent increase.





 Alcohol
Alcohol

